Spider Veins
Overview
What are spider veins?
What Are the Common Causes of Spider Veins?
The primary goal of leg veins is carrying blood up towards the heart, resisting the gravitational pull. This can be accomplished because of vein valves, flap-like components within your veins that act as one-way doors — they allow blood to flow towards the heart but prevent it from flowing back down.
Chronic venous insufficiency is a medical condition wherein your vein valves collapse and malfunction due to various factors, making blood flow backward due to gravitational force. Over time, blood continues accumulating in your leg veins, placing extreme pressure on your vein walls, eventually leading to spider veins.
Are there any symptoms of spider veins?
However, the underlying vein disease can cause numerous symptoms, including leg heaviness, restless leg syndrome, throbbing leg veins, frequent muscle cramps, aching, itching, and tingling sensations. These symptoms usually worsen at the end of the day or after long periods of sitting or standing still.
If left untreated, the underlying vein disease can also lead to skin changes, discoloration, non-healing leg wounds (ulceration), and deep vein thrombosis. As such, you must contact a spider vein treatment center in California at an early stage to diagnose the root cause of spider veins.
What are the risk factors for spider veins?
Sex is the second biggest risk factor for spider veins — approximately 54% of women and 45% of men in the United States experience symptoms of vein disease. This is because higher levels of estrogen increase your risk of spider veins, which means you also have a higher risk if you’re pregnant, taking birth control pills, or undergoing hormone therapy.
Age is an important risk factor for spider veins — your vein valves weaken as you grow older, increasing the risk of spider veins and vein disease.
Other risk factors for spider veins include obesity, leg injuries, a history of blood clots, or if you sit or stand for long periods because of your job.
How do your vein doctors in California treat spider veins?
Without underlying vein disease, it’s not necessary to treat spider veins, though you can still opt for sclerotherapy sessions to improve your legs’ cosmetic appearance.
However, if you have underlying vein disease, seeking prompt vein treatment in California is crucial. If you get spider vein treatments without addressing the underlying problems, you’ll probably experience a recurrence. Our vein doctors always treat the underlying vein disease and the superficial vein problems, ensuring holistic and optimal results.
How Do New Jersey Vein Clinics Treat Spider Veins?
What are the best spider vein treatments in California?
Sclerotherapy:
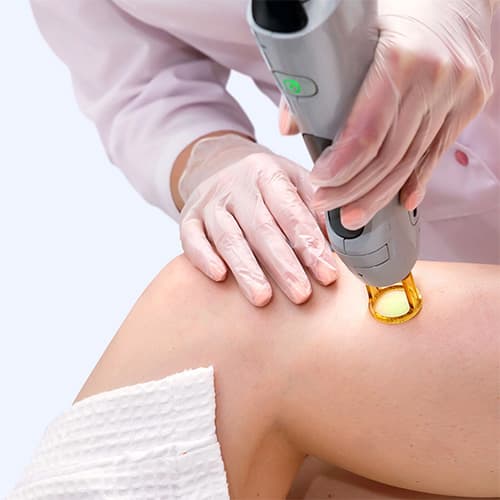
Endovenous Laser Ablation:
Radiofrequency Ablation:

Laser Therapy:

Compression Stockings:
